While trail running shoes can be used on roads, especially in situations where a runner encounters mixed terrains or pref...
The Daily Run
Join over 10,000 subscribers that receive running routines, motivation, tools, playlists & giveaways. Sent to your inbox every day.

Latest Articles
Read All Articles Is It OK to Use Trail Running Shoes on the Road?
Is It OK to Use Trail Running Shoes on the Road? Is Running on a Treadmill Easier Than Running Outside?Runners have their own preferences, whether it is treadmill running, running outside on the road, or exploring trails. So...
Is Running on a Treadmill Easier Than Running Outside?Runners have their own preferences, whether it is treadmill running, running outside on the road, or exploring trails. So...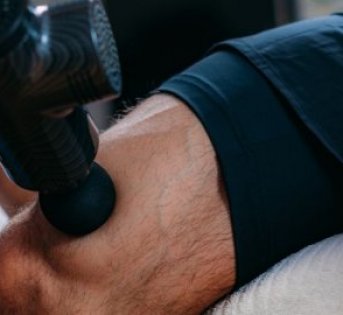 How to Fix Sore Quads After Running?Rest, ice, gentle stretching, and over-the-counter pain relievers can help soothe sore quads after running. Also, ensure ...
How to Fix Sore Quads After Running?Rest, ice, gentle stretching, and over-the-counter pain relievers can help soothe sore quads after running. Also, ensure ... 10 Fruits With The Most Electrolytes to Replace Sports DrinksThese fruits are high in electrolytes such as potassium, magnesium, and calcium, essential for hydration, muscle function...
10 Fruits With The Most Electrolytes to Replace Sports DrinksThese fruits are high in electrolytes such as potassium, magnesium, and calcium, essential for hydration, muscle function...
The Passionate Runner Podcast
Trending
RunnerClick Voices
Pam Berg
Running Coach
Megan Robinson
Sports Dietician
Evan Wood
RRCA Level 1 Running Coach
Whitney Heins
VDOT-02 Running Coach
RunnerClick is setting the pace
Run by runners, for runners. We pride ourselves on the depth of research, quality and transparency we put into every article, review, and buying guide.
More About RunnerClick- All product recommendations are thoroughly tested to ensure reviews and buying guides are of the highest caliber.
- All health, injury and training topics are medically reviewed by doctors, trainers and subject matter experts.
- From medical research, new product launches and industry trends, our writers and subject matter experts continually monitor the running space.




















